Fertility Assessments for women
At LifeSure, we offer a fertility assessment for women who wish to assess their level of fertility.
This includes:
Anti-Müllerian Hormone (AMH) blood test: This measures the level of AMH in your blood and provides an accurate indication of your ovarian reserve level.
Pelvic ultrasound scan: Otherwise known as a transvaginal or gynaecological scan , this test uses ultrasound imaging to examine the health of the ovaries, womb and fallopian tubes.
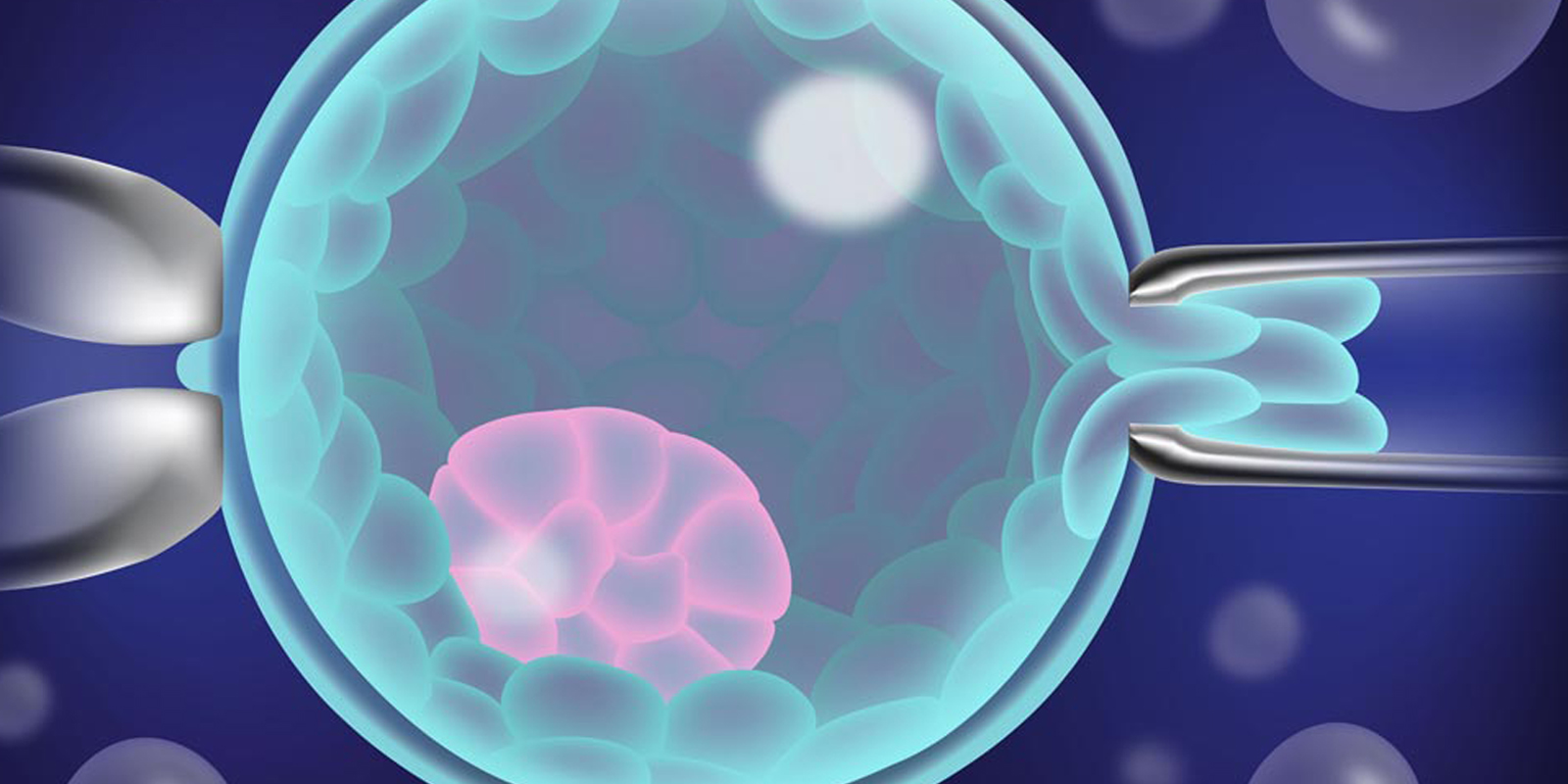
Mock embryo transfer: This procedure allows your consultant to select the most effective route and location for embryo transfer if you are considering IVF treatment.
Your consultation with one of our fertility specialists: Included with your Diagnostic Pack is your initial consultation where you will meet with your doctor to discuss the most effective fertility treatment options based on your results.
Causes of female infertility
The main causes of female factor infertility include advanced maternal age , ovulation disorders and partial or complete blockages within the fallopian tubes.
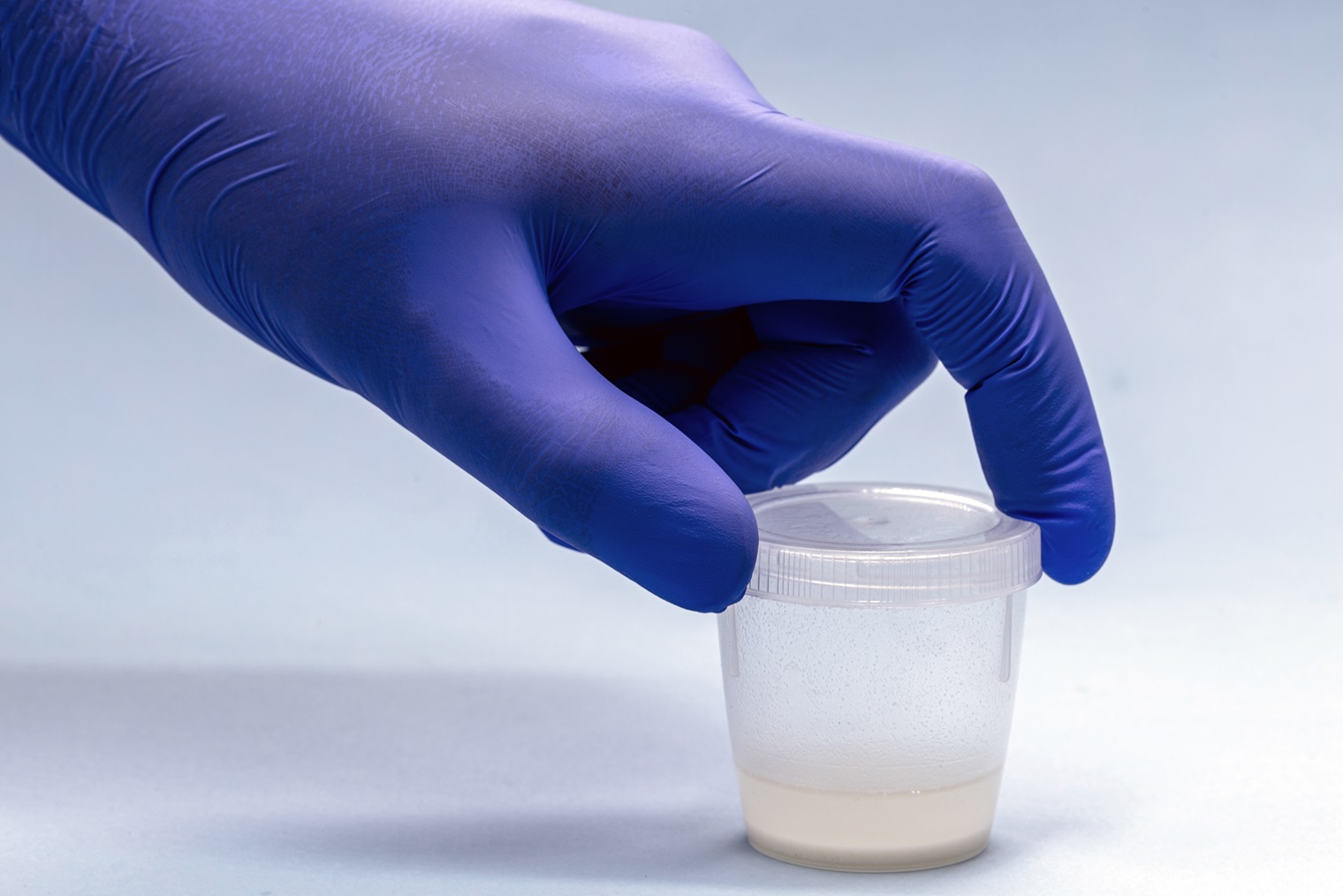
Fertility Assessments for men
The most common cause of male factor infertility is due to semen abnormalities. For men, a fertility assessment involves a semen analysis, otherwise known as a seminogram. During a semen analysis, a semen sample is analysed to establish the sperm count (the number of sperm present), sperm motility (how the sperm move) and sperm morphology (the shape of the sperm).
In some cases, sperm quality is affected by certain lifestyle factors, such as drinking alcohol, smoking or being overweight. Your consultant can discuss your results with you and advise whether changing lifestyle habits could increase your potential to conceive.
Fertility Assessments for couples
For couples, we offer a complete fertility assessment package called the Diagnostic Pack Plus. Unlike the Diagnostic Pack which is designed to assess female fertility, the Diagnostic Pack Plus includes fertility assessments for both partners. It is suitable for couples who are seeking fertility treatment and couples who may wish to start a family and want to gain a clear picture of their fertility for the future. It includes:
- Your consultation with one of our fertility specialists
- Medical assessments for both you and your partner
- Anti-Müllerian Hormone (AMH) blood test
- Pelvic ultrasound scan
- Mock embryo transfer
- Semen analysis
Answer the questions below to discover your female infertility risk factors.
Take this personal risk assessment to help you understand what the underlying causes of your infertility might be.
Are you over age 35?
Age is an important infertility risk factor, yet one that you cannot control. After age 35, a woman’s fertility potential starts to decline. Then after age 40, the chance of getting pregnant sharply declines. The aging process decreases the number of eggs you have, as well as makes the eggs more susceptible to chromosomal abnormalities. Women over 35 have a higher chance of miscarriage, too.
Do you smoke?
Are you overweight?
Fortunately, your weight is typically one fertility risk factor that you can change. Just a BMI (body mass index) 10 to 15 percent above normal can lead to higher levels of estrogen in your body that can disrupt normal ovulation. Additionally, overweight women often have excessive amounts of androgens, as well as insulin, which can disrupt ovulation and make it hard to get pregnant.
Are you underweight or have an eating disorder?
On the flip side, women who are underweight are often hypo-estrogenic, which means they don’t produce enough estrogen to ovulate normally. Underweight women are unable to produce the necessary hormones to trigger ovulation, which is essential for conception. Eating disorders, such as anorexia and bulimia, can also lead to abnormal menstrual cycles and infertility. It’s best to seek professional help right away if you suffer from either condition.
Do you exercise excessively?
Do you have a history of sexually transmitted diseases (STDs)?
STDs such as gonorrhea and Chlamydia are common infertility risk factors that can lead to pelvic inflammatory disease (PID) if left untreated. PID can result in complications such as scarring, miscarriage, ectopic pregnancy, and blocked fallopian tubes – all of which can adversely affect your chances of getting pregnant.
Do you have irregular periods or experience bleeding or spotting between periods?
Ovulation is essential to getting pregnant. If you don’t have a period, or if your cycles are more than 35 days apart or less than 25 days apart, you may have an ovulatory disorder, one of the leading causes of infertility. Even if you do experience normal periods, you still may have problems ovulating. Abnormal bleeding or spotting between periods should also be taken into consideration as part of your infertility risk assessment. Any sort of unexplained bleeding could signal hormonal problems, fibroids, polyps, or uterine or cervical problems.
Do you experience pain during your periods or sexual intercourse?
Pelvic pain may indicate endometriosis, tubal disease, pelvic inflammatory disease, or fibroids, all of which can negatively affect fertility.
Do you have a history of recurrent miscarriage?
Recurrent miscarriages may be caused by structural abnormalities of the uterus or uterine fibroids. A uterine infection, low hormone levels or a dysfunction of the immune system can also trigger multiple miscarriages.
Do you drink excessive amounts of coffee or alcohol or use illicit drugs?
If you answered “yes” to any of these questions, your fertility might be at risk.
Answer the questions below to discover your male infertility risk factors.
What are a man’s risk factors for infertility? Take this personal male fertility risk assessment to help you understand what the underlying causes of your infertility might be.
Do you smoke cigarettes or marijuana or use illicit drugs?
Have you experienced prior trauma to your testicles or have you noticed physical changes in the pelvic region?
A history of scrotal or pelvic trauma or a spinal injury can limit a man’s ability to produce sperm or get an erection. Similarly, anatomical issues, such as a testicular mass or a varicocele (a group of dilated veins draining the testicle) should raise a red flag. Further, previous surgery, cystic fibrosis, or certain types of birth defects can cause a blockage in the tubes that carry sperm from the testicles to the penis, causing infertility.
Do you have a chronic health condition?
Chronic medical conditions may cause potential problems with conception. Medical conditions that can affect male fertility include diabetes, HIV, thyroid disease, Cushing syndrome, heart attack, liver or kidney failure, and chronic anemia. Certain types of medications taken for these and other medical conditions can also impair sperm production, such as medicines for ulcers, psoriasis, depression, and high blood pressure.
Do you have a history of sexually transmitted diseases or other infections of the genital?
Repeated STD infections, such as Chlamydia or gonorrhea, are most often associated with male infertility by causing scar tissue and blocking sperm passage. Human papilloma viruses (HPV), the cause of genital warts, may also impair sperm function. Non-STD infections that may affect fertility include prostatitis (inflammation in the prostate gland), orchitis (in the testicle), semino-vesculitis (in the glands that produce semen), or urethritis (in the urethra), perhaps by altering sperm motility. Even after successful antibiotic treatment, infections in the testes may leave scar tissue that blocks the passage of sperm.
Are you overweight?
Obesity may impair hormonal levels and adversely affect fertility. Fortunately, your weight is typically one fertility risk factor that you can change.
Are you exposed to toxic chemicals or heavy metals on a regular basis?
Occupational or other long-term exposure to certain types of toxins and chemicals (such as herbicides and pesticides) may reduce sperm count by either affecting testicular function or altering hormone systems. Estrogen-like and hormone-disrupting chemicals such as bisphenol A, phthalates, and organochlorines are particular potential concerns. Chronic exposure to heavy metals such as lead, cadmium, or arsenic may affect sperm quality. These chemicals generally affect men who have long-term and intense exposure to them.
Do you ride bicycles frequently?
Do you use performance enhancing drugs, such as testosterone or steroids?
Anabolic steroids used to enhance strength and fitness can actually drastically lower a man’s sperm count, sometimes even to zero in many cases. Similarly, testosterone supplements can also cause sperm counts to plummet.
Do you have a history of cancer?
Certain cancers, particularly testicular cancer, impair sperm production, often severely. Cancer treatments such as chemotherapy and radiation can damage sperm quality and quantity, causing infertility. The closer radiation treatments are to reproductive organs, the higher the risk for infertility.
If you answered “yes” to any of these questions, your fertility might be at risk.